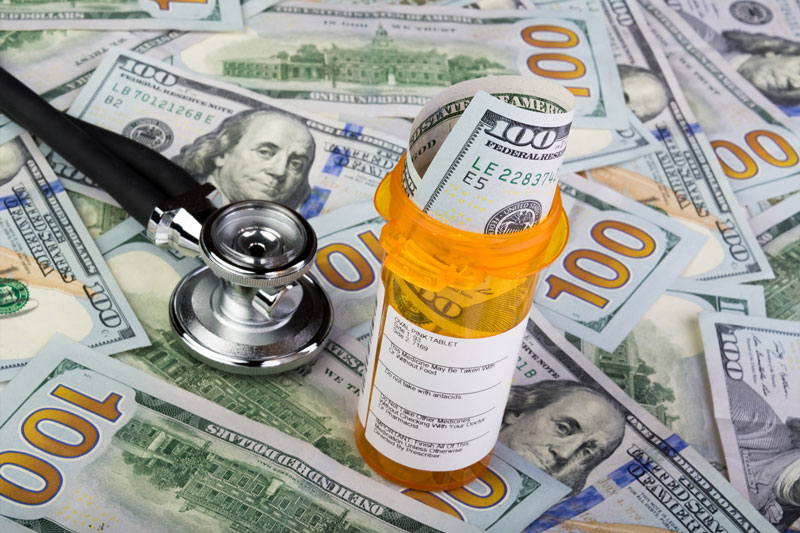
A new report from the Government Accountability Office has revealed that under the Affordable Care Act (Obamacare), hospitals received thousands of dollars in bonuses even though they had significantly low quality scores.
The new report appears to be the latest in a series which have essentially exposed the flaws in the Obamacare program.
Initiated under Obamacare, the Hospital Value-Based Purchasing scheme was shaped in a way that it incentivized hospitals in order to effectively increase the quality of healthcare being offered and also increase efficiency.
While the scheme was supposed to reward hospitals that provided high quality medical care at lower costs, auditors at the agency discovered that hospitals that had high efficiency scores but offered drastically low quality continued to receive bonuses.
“While a majority of all hospitals received a bonus or a penalty of less than 0.5 percent each year, the percentage of hospitals receiving a bonus greater than 0.5 percent increased from 4 percent to 29 percent from fiscal year 2013 to 2017,” the report states.
It was found that in fiscal year 2017, hospitals that received a bonus even though their quality scores were well below the median, numbered 345. Additionally, auditors also found that from 2015 through 2017, almost 20 percent of all hospitals that received a bonus for maintaining high quality, had a below average quality score.
The report goes on to state that in fiscal year 2017, the average bonus awarded to all hospitals was $67,511. It should come as no surprise that this is more than double amount awarded to hospitals in 2013 when the average bonus hospitals received was $30,352.
Furthermore, it was also discovered that if a hospital did not have quality scores due to some reason, it would make their efficiency scores even higher, and because of how the agency calculated the score, such hospitals were more likely to be awarded a bonus.
“In fiscal year 2017, 68 percent of hospitals with missing domain scores received a bonus, compared to 50 percent of hospitals with all domain scores,” the report explains. “For example, in fiscal year 2017, 182 of the 345 lower quality hospitals that received a bonus (53 percent) were missing at least one quality domain score.”
“CMS signaled the importance of hospitals’ providing care at a lower cost to Medicare, and, in its weighting formula, the agency tried to find balanced consideration for quality and cost,” the report states. “Rather than achieving this balance—which would have allowed the agency to identify and reward higher quality and lower cost hospitals—CMS’s weighting formula has resulted in bonuses for some lower quality hospitals, solely due to their cost efficiency.”
Following the release of the report, the agency announced that it is considering changing the way it currently calculates the scores.
“HHS is committed to improving the quality of care across settings while also improving the efficiency of care and patient experience,” said Barbara Clark, acting assistant secretary for legislation at the agency. “HHS will examine alternatives and consider revising the formula for the calculation of hospitals’ [total performance score] consistent with relevant statutory guidance, and in a way to reduce the effect of the efficiency domain on the [total performance score].”